New study shows link between long-term exposure to air pollution and liver disease

A large-scale epidemiologic study in China has identified links between long-term exposure to ambient air pollution and metabolic-associated fatty liver disease (MAFLD), report scientists in the Journal of Hepatology.
Amsterdam, December 6, 2021 – Metabolic-associated fatty liver disease (MAFLD) is a growing global health challenge and poses a substantial economic burden. A large-scale epidemiologic study in China has identified links between long-term exposure to ambient air pollution and MAFLD. These links are exacerbated by unhealthy lifestyles and the presence of central obesity, report scientists in the Journal of Hepatology, the official journal of the European Association for the Study of the Liver, published by Elsevier.
The incidence of MAFLD has increased steadily since the 1980s, currently affecting a quarter of the global population and a majority of patients with adult-onset diabetes and poses a substantial global burden. In Asia, MAFLD increased to 40% between 2012 and 2017. Formerly known as non-alcoholic fatty liver disease (NAFLD), it may progress to end-stage liver diseases such as cirrhosis and liver cancer, liver transplantation and liver-related death.
Accumulating animal studies have shown that breathing air pollutants may increase the risk of MAFLD. For instance, fine particulate matter exposure may trigger a non-alcoholic steatohepatitis (NASH)-like phenotype, impair hepatic glucose metabolism, and promote hepatic fibrogenesis.
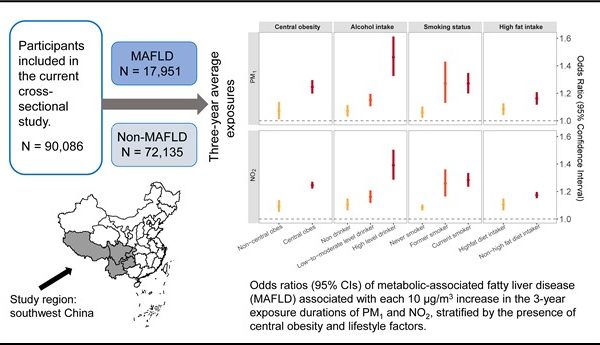
Caption: A large-scale epidemiologic study in China has identified links between long-term exposure to ambient air pollution and metabolic-associated fatty liver disease (MAFLD) (Credit: Journal of Hepatology).
The MAFLD epidemic corresponds to environmental and lifestyle changes that have occurred alongside rapid industrialisation worldwide, especially in many Asian countries,
explained lead investigator Dr Xing Zhao, West China School of Public Health and West China Fourth Hospital, Sichuan University, Chengdu, Sichuan, China.
A growing number of studies have suggested that ambient air pollution, which is the biggest environmental problem caused by industrialisation, may increase the risk of metabolic disorders such as insulin resistance and dyslipidaemia, and related diseases, such as type 2 diabetes mellitus and metabolic syndrome. However, epidemiologic evidence for the association was limited, so we conducted this research to improve our understanding of the effects of air pollution on human health and also to help reduce the burden of MAFLD.
Investigators conducted an epidemiologic study on the potential role of ambient air pollution in the risk of MAFLD in approximately 90,000 adults in China based on the baseline survey of the China Multi-Ethnic Cohort (CMEC), a prospective cohort that enrolled nearly 100,000 participants in south-west China from 2018 to 2019. The CMEC collected participant information including sociodemographics, lifestyle habits, and health-related history through verbal interviews performed by trained staff and subsequently assessed anthropometrics, biosamples (blood, urine, and saliva), and imaging data.
Researchers found that long-term exposure to ambient air pollution may increase the odds of MAFLD, especially in individuals who are male, smokers, and alcohol drinkers, and those who consume a high-fat diet. Unhealthy lifestyle behaviours and an excess accumulation of fat in the abdominal area may exacerbate the harmful effects.
Our findings add to the growing evidence of ambient pollution’s damaging effects on metabolic function and related organs. However, physical activity did not seem to modify the associations between air pollution and MAFLD. We suggest that future studies explore whether the timing, intensity, and form of physical activity can mitigate the harmful effects of air pollution,
commented Dr Zhao and his co-investigators.
The investigators propose that air pollution should be recognised as a modifiable risk factor for MAFLD. Populations at high risk should be aware of the air quality in the areas where they live and plan their activities to minimise their exposures to air pollution.
In an accompanying editorial, Dr Massimo Colombo, San Raffaele Hospital, Liver Center, Milan, Italy, and Dr Robert Barouki, University of Paris, Inserm Unit T3S, Paris, France, noted that the assessment of the major determinants of mortality worldwide by WHO showed that global pollution topped the list, ranking higher than smoking, alcohol consumption, and major infectious diseases, and that air pollution, the most critical component of global pollution, is likely to be responsible for millions of deaths per year worldwide.
A better characterisation of the liver exposome is expected to improve prevention and precautionary counselling. Indeed, whereas physical activity together with a healthy diet stand as a primary pillar in the fight against metabolic syndrome associated morbidities, including MAFLD, the findings that ambient pollution could exacerbate MAFLD risk might offer new clues to refining the counselling of these patients, for instance by restricting exposure of risk populations to open air settings at high levels of pollution, as is recommended for patients suffering from severe asthma. It also constitutes an additional incentive for decision-makers to speed up the efforts to conform with the WHO guidelines and limits on air pollution, as many cities in Europe and worldwide are still well above those limits,
commented Dr Colombo and Dr Barouki.
Notes for editors
The article is “Exposure to air pollution is associated with an increased risk of metabolic dysfunction-associated fatty liver disease,” by Bing Guo, Yuming Guo, Qucuo Nima, Yuemei Feng, Ziyun Wang, Rong Lu, Baimayangji, Yue Ma, Junmin Zhou, Huan Xu, Lin Chen, Gongbo Chen, Shanshan Li, Huan Tong, Xianbin Ding, and Xing Zhao on behalf of the China Multi-Ethnic Cohort (CMEC) collaborative group (https://doi.org/10.1016/j.jhep.2021.10.016). The editorial is “Expanding the liver exposome: should hepatologists care about air pollution?” by Massimo Colombo and Robert Barouki (https://doi.org/10.1016/j.jhep.2021.11.001). They will appear online in advance of the Journal of Hepatology, volume 76, issue 3 (March 2022) published by Elsevier.
The article is openly available at https://www.journal-of-hepatology.eu/article/S0168-8278(21)02153-X/fulltext and the editorial at https://www.journal-of-hepatology.eu/article/S0168-8278(21)02165-6/fulltext.
This study was supported by the National Key R&D Program of China (2017YFC0907305), the Natural Science Foundation of China (81973151, 81773548), and China Postdoctoral Science Foundation (2020M68335).
Full text of this article and editorial is available to credentialed journalists upon request; contact Vicki Wetherell at +44 1865 843193 or hmsmedia@elsevier.com. Journalists wishing to interview the study authors should contact Dr Xing Zhao at xingzhao@scu.edu.cn. To reach the authors of the editorial for comment, please contact Massimo Colombo at mcolombo46@yahoo.it.
About the Journal of Hepatology
The Journal of Hepatology, the premier journal devoted to liver diseases, is the official journal of the European Association for the Study of the Liver (EASL). It publishes original papers, reviews, case reports, and letters to the Editor concerned with clinical and basic research in the field of hepatology. The journal has a 2020 Impact Factor of 25.083 (Source: Journal Citation ReportsTM from Clarivate, 2021).
About EASL
In the fifty plus years since EASL was founded, it has grown from a small organisation that played host to 70 participants at its first meeting, to becoming the leading international liver association. EASL attracts the foremost hepatology experts as members and has an impressive track record in promoting research in liver disease, supporting wider education, and promoting changes in European liver policy.
About Elsevier
As a global leader in information and analytics, Elsevier helps researchers and healthcare professionals advance science and improve health outcomes for the benefit of society. We do this by facilitating insights and critical decision-making for customers across the global research and health ecosystems.
In everything we publish, we uphold the highest standards of quality and integrity. We bring that same rigour to our information analytics solutions for researchers, health professionals, institutions and funders. Elsevier employs 8,100 people worldwide. We have supported the work of our research and health partners for more than 140 years. Growing from our roots in publishing, we offer knowledge and valuable analytics that help our users make breakthroughs and drive societal progress. Digital solutions such as ScienceDirect, Scopus, SciVal, ClinicalKey, and Sherpath support strategic research management, R&D performance, clinical decision support, and health education. Researchers and healthcare professionals rely on our 2,500+ digitised journals, including The Lancet and Cell; our 40,000 eBook titles; and our iconic reference works, such as Gray’s Anatomy. With the Elsevier Foundation and our external Inclusion & Diversity Advisory Board, we work in partnership with diverse stakeholders to advance inclusion and diversity in science, research and healthcare in developing countries and around the world.
Elsevier is part of RELX, a global provider of information-based analytics and decision tools for professional and business customers.